
This meta-analysis explored the link between work injuries and mental health challenges.
Providing background:
· A large number of people “endure preventable work injuries and manageable mental health conditions”, and these issues are compounded by “widespread underreporting, driven by fears of repercussions, insufficient workplace accommodations, and complex reporting processes”
· There’s limited consensus regarding the magnitude and direction of the relationship between mental health challenges and work injuries
· Most studies are said to assume that work injuries precede mental health challenges, but another stream of research assumes the opposite relationship
· This work draws on ‘uncertainty in illness’ theory, which states that “people struggle to find meaning when confronted with illness-related events or stimuli, such as acute work injuries or ongoing mental health challenges”
· The broader concept of mental health includes state and variation of an individual’s psychological well-being and distress, with a “complete state” encompassing healthy cognitive, emotional and social functioning; mental health challenges “arise from prolonged deviations from this state”
The studies hypotheses were:
· There will be a positive association between prior work injuries and subsequent mental health challenges.
· There will be a positive association between prior mental health challenges and subsequent work injuries.

Results
Key findings were that:
· There’s a consistent and modest link between work injuries and mental health challenges
· The relationship is stronger when work injuries precede mental health challenges compared to the reverse
· Hence, mental health challenges were more likely to follow from work injury than work injury to follow from mental health challenges
· Negative cognitions and perceived job demand underpin the bidirectional relationship
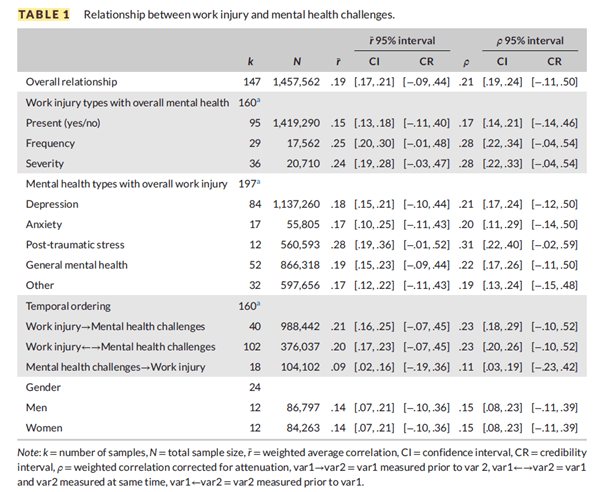
Discussing the findings, it’s said that studies that measured work injuries prior to or simultaneously with mental health challenges demonstrated larger effect sizes compared to studies that measured work injuries following the assessment of mental health challenges.
While this doesn’t demonstrate a causal relationship, the findings “align with the uncertainty in illness theory (Mishel, 1988, 1990) and suggest that mental health challenges are more likely to follow work injuries rather than precede them”.
They say that this contributes evidence to the idea that mental health challenges can be anticipated as a potential consequence of work injuries, it also highlights that “mental health challenges may serve more as distal antecedents of work injuries, influenced by various factors resulting from mental health challenges and more proximal to work injuries”.
Two malleable factors were found to underlie the bidirectional relationship. First, negative cognitions, like rumination, mediate the relationship between between work injuries and mental health challenges.
Perceived job demands was another significant mediator, linked to coping with mental health challenges to work injuries. The effect of perceived job demands was relatively weaker, “possibly due to work modifications or time away from work that often arises because of these issues”.
The nature of the work itself also influenced the relationship, as did the severity and frequency of injuries having a stronger association with mental health challenges than just the presence of a work injury.
They talk about the limitations of how some studies dichotomised the capture of health health challenges (e.g. ‘depressed’ vs ‘not depressed’), and how this affects variance in these variables and results in smaller average effect sizes; and hence “potentially impacting comparisons between types of mental health challenges due to this analytical approach”.
Dichotomising mental health challenges and work injuries is argued to also lead to other concerns. For one, while it may be pragmatic to use established clinical cut-offs or capture injury via analytical assumptions, the findings highlight the need for improved measurement and reporting of mental health challenges and work injuries.
Gender wasn’t found to moderate the relationship in this study – suggesting that gender either doesn’t influence the relationship, or “or the complexities of considering gender—as men tend to experience more work injuries (Smith &Mustard, 2004; Stergiou-Kita et al., 2015) and women exhibit higher levels of depression (Hyde et al., 2008; Salk et al., 2017)—might obscure any potential differences”.
Age, education, marital status, tenure, work status and income also didn’t influence the relationship.
However, the proportion of visible minorities in a sample showed a moderating effect on the relationship between work injuries and mental health challenges, such that a higher proportion of minorities was associated with a stronger relationship.
An extensive body of research highlights health disparities among minorities, with evidence suggesting that they are more susceptible to work injuries and mental health challenges.

Granger, S., & Turner, N. (2024). Work injuries and mental health challenges: A meta‐analysis of the bidirectional relationship. Personnel Psychology.
Study link: https://onlinelibrary.wiley.com/doi/pdf/10.1111/peps.12649
My site with more reviews: https://safety177496371.wordpress.com
LinkedIn post: https://www.linkedin.com/pulse/work-injuries-mental-health-challenges-meta-analysis-ben-hutchinson-tubac
One thought on “Work injuries and mental health challenges: A meta-analysis of the bidirectional relationship”